- Your cart is empty
- Continue Shopping
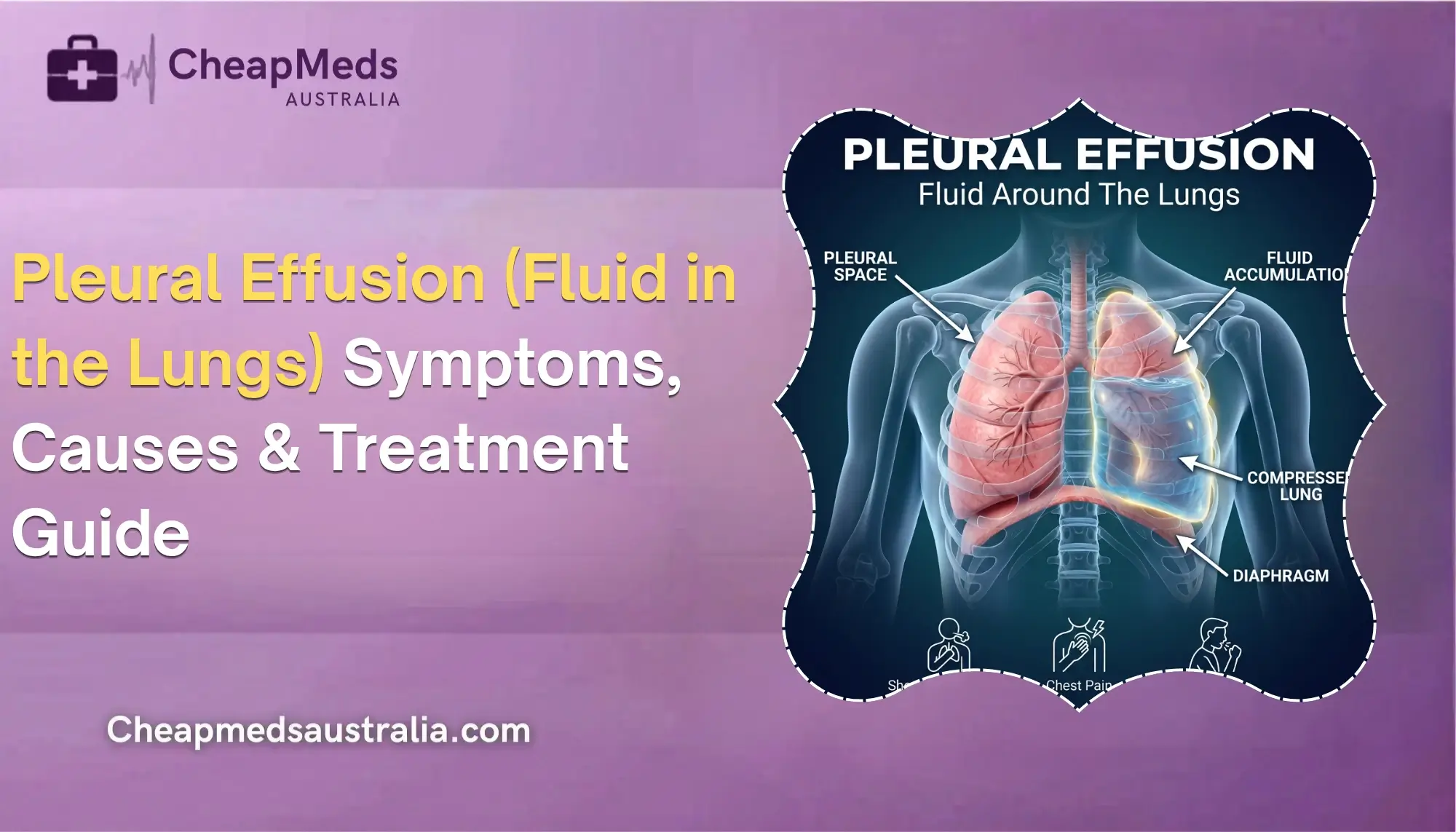
Pleural Effusion (Fluid in the Lungs): Symptoms, Causes & Treatment Guide
Have you ever felt short of breath without any obvious reason? Or did you have a dull, constant pain in your chest that wouldn’t go away? Sometimes, a little trouble breathing can mean something worse, such as fluid building up around your lungs.
This condition is known as pleural effusion, and while the name might sound intimidating, understanding it can make a real difference in how quickly someone gets the right help.
What Is Pleural Effusion?
Your lungs are surrounded by a thin two-layered membrane called the pleura. A small space, the pleural space, exists between these two layers and usually contains a thin layer of fluid. This fluid is similar to a lubricant that works on your lungs — allowing them to open and close seamlessly every time you breathe.
But when this space fills with too much fluid, it forms what doctors call a pleural effusion, meaning that there is fluid in the lungs’ heavy outer covering. The extra fluid exerts pressure on the lungs, making it more difficult to take a normal breath.
It’s worth knowing that pleural effusion isn’t a disease on its own. It’s your body’s way of reacting to something else going wrong — and figuring out what that something is is really the whole point of treatment.
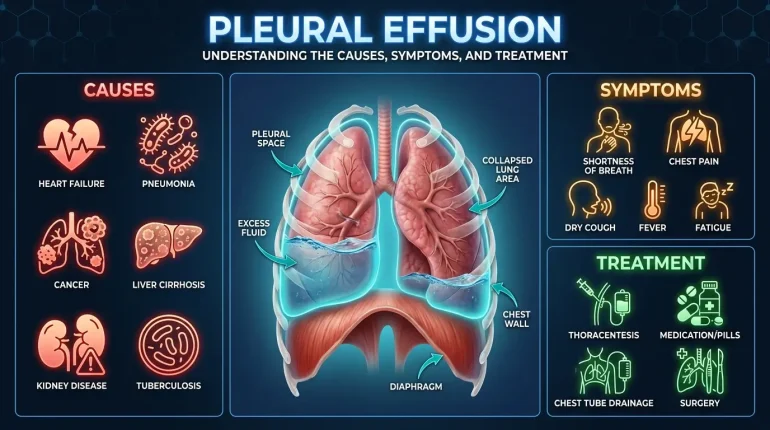
What Causes Fluid to Build Up in the Lungs?
Fluid can accumulate around the lungs for many different reasons. Doctors typically separate these into two broad categories: transudative and exudative effusions.
Transudative Pleural Effusion
This type happens when fluid is essentially pushed or squeezed out of the blood vessels into the pleural space, usually because of pressure problems or low protein levels in the blood. The most common causes include:
- Congestive heart failure — the most common cause overall. When the heart struggles to pump blood efficiently, fluid starts backing up and can leak around the lungs.
- Liver cirrhosis — damage to the liver can cause fluid to migrate from the abdomen into the chest cavity.
- Kidney disease or nephrotic syndrome — when the kidneys aren’t filtering properly, protein levels in the blood drop, and fluid distribution in the body goes off balance.
Browse our Azithromycin treatment options commonly used for bacterial chest infections and respiratory conditions that may affect lung health.
Exudative Pleural Effusion
This type involves inflammation, infection, or abnormal tissue that causes fluid to leak directly into the pleural space. Common causes here include:
- Pneumonia — a serious lung infection that can inflame the pleural lining and set off fluid buildup.
- Cancer — lung cancer, breast cancer, and lymphoma are among the cancers most likely to cause what doctors call a malignant pleural effusion.
- Pulmonary embolism — a blood clot that gets lodged in the lungs.
- Tuberculosis (TB) — still one of the leading causes in developing countries.
- Autoimmune diseases — conditions like lupus or rheumatoid arthritis can trigger inflammation in the pleural lining.
Pleural Effusion Symptoms: Signs of Fluid in the Lungs
Here’s something that catches a lot of people off guard — small effusions often cause no symptoms whatsoever. You could have a minor fluid buildup and feel completely fine. Symptoms tend to show up only once enough fluid has accumulated to actually interfere with how your lungs work.
Here are the most common pleural effusion symptoms to watch for:
Shortness of Breath
This is the hallmark symptom. Fluid collects in the cavity, compressing the lung against the chest wall and impeding breathing. It may be something that you first notice on exertion, but the effusion can develop to cause breathlessness at rest.
Chest Pain or Pressure
There is a feeling of heaviness, discomfort or tightness in the chest. Some simply write it off as a feeling of something pressing down on one side. Sometimes, the pain may be intense, particularly with deep breaths — this is called pleuritic chest pain.
Persistent Dry Cough
Fluid in the lungs can cause a cough that is not initially linked to anything specific and does not respond to common cough syrups.
Experiencing breathing discomfort or chest congestion? Explore AB Phylline 200 mg for respiratory support treatment options.
Fever and General Discomfort
If the effusion is due to an infection or inflammation, you may also have fever, chills and a general feeling of being unwell.
Symptoms of the Underlying Cause
Pleural effusion is usually a complication of another disease, and you may identify the accompanying symptoms that fluid in the lungs brings with those caused by the primary illness — swelling in the leg due to heart congestion, night sweats due to TB.
NOTE: If you have unexplained breathlessness or chest pain, please do not take this lightly. Always get medical care to exclude serious disease.
How Is It Diagnosed?
If a doctor suspects pleural effusion based on your symptoms, they’ll typically use a combination of:
- Physical examination — listening to the lungs with a stethoscope may reveal dullness or absent breath sounds on one side.
- Chest X-ray — typically the starting point. Even moderate amounts of fluid show up clearly on an X-ray.
- Ultrasound — excellent at spotting even small amounts of fluid, and very useful for guiding any procedures that follow.
- CT scan — gives a more detailed look at what’s happening and often helps identify the underlying cause.
- Thoracentesis — in many cases, actually removing and testing some of the fluid is the only reliable way to confirm whether it’s transudative or exudative, and to get closer to understanding why it’s there.
Treatment Options for Pleural Effusion
Treatment depends entirely on the underlying cause and how much fluid has built up. The goal is twofold: remove the excess fluid to relieve symptoms, and treat the root condition to prevent it from coming back.
1. Treating the Underlying Cause
In many patients, effectively treating the underlying condition (e.g., heart failure, infection, or an autoimmune disease) resolves the effusion. In less severe cases where small amounts of water build up in the space surrounding the lungs, physicians may just observe and wait.
2. Thoracentesis
When the fluid is causing significant discomfort or breathing difficulties, thoracentesis is often the most immediate treatment. It is a minimally invasive procedure in which a doctor uses a thin needle or small catheter and inserts it through the chest wall to directly access and remove pleural fluid.
It’s usually done under local anaesthesia with ultrasound guidance, and the whole thing usually takes between 15 and 30 minutes. Most patients notice the difference almost straight away — breathing gets easier and that heavy chest pressure lifts. The fluid that’s removed is sent to a lab to help pin down the cause.
While thoracentesis is generally safe, it does carry some small risks, including pneumothorax (air entering the pleural space) and minor bleeding, which your doctor will discuss with you beforehand.
3. Chest Tube Drainage (Tube Thoracostomy)
For more massive or complicated effusions, especially if from infection (empyema), a chest tube may be placed and kept in place for several days to allow gradual drainage of fluid.
4. Pleurodesis
If the effusion keeps recurring, a procedure called pleurodesis may be recommended. A special substance (usually talc) is introduced into the pleural space to cause the two layers to stick together, eliminating the space where fluid can collect.
5. Surgery
If other treatments have failed or if you have a cancer-related effusion, a surgical procedure can also sometimes be used (but this is rare). This may involve the insertion of an indwelling pleural catheter, allowing patients to drain fluid at home on a regular basis.
Experiencing chest tightness or discomfort along with breathing issues? Discover pain management products that may help support comfort during recovery.
When Should You See a Doctor?
See a doctor right away if you have any of these:
- Sudden or worsening shortness of breath
- Pain in your chest, especially if it gets worse when you take a deep breath
- An unexplained cough for a while
- Fever alongside breathing difficulty
- A fast heart rate associated with any of the above
Early diagnosis can make a significant difference, not just in treating the effusion itself, but in catching any serious underlying condition before it progresses.
Can Pleural Effusion Be Prevented?
Since pleural effusion is commonly associated with other medical conditions, not all cases can be avoided. Yet, the right habits along with medical care can truly decrease this risk.
Let us now take a look at some of the preventive measures:
- Manage chronic conditions proactively — if you have heart disease, kidney issues, or liver disease, adhere to your treatment plan so that it lowers the risk for fluid imbalances, causing effusion.
- Treat respiratory infections early — don’t leave pneumonia or other chest infections untreated. Prompt antibiotic therapy can prevent complications, including fluid buildup.
- Quit smoking — smoking results in lung tissue damage, which can lead to infections and lung cancer that are associated with pleural effusion.
- Avoid exposure to harmful substances — asbestos and certain environmental toxins are directly linked to pleural disease. If your work environment puts you at risk, protective equipment isn’t optional.
- Stay on top of routine health check-ups — regular screenings catch things early, before they become serious enough to cause complications like effusion.
A proactive approach to your overall health is one of the best defences against conditions like pleural effusion.
Struggling with breathing discomfort or chest tightness? Explore our respiratory care category for supportive treatment options.
Living With Pleural Effusion
For the majority of people, once the effusion is drained and the underlying condition is being managed, everyday life returns to normal fairly quickly. That said, conditions like advanced heart failure or certain cancers may mean ongoing monitoring and periodic drainage appointments become part of your routine.
Staying connected with your medical team, keeping follow-up appointments, and flagging any new or worsening symptoms early, that’s really the foundation of managing this well long-term.
Frequently Asked Questions
1. What is pleural effusion?
Pleural effusion happens when too much fluid builds up in the area around the lungs, making it hard to breathe. Underlying health problems, such as an infection, heart failure, or lung illness, often cause it.
2. What are the common pleural effusion symptoms?
A dry cough, chest pain, shortness of breath, and a sense of pressure in the chest are all signs that you might have pleural effusion. As more fluid builds up, the symptoms may get worse.
3. What causes fluid in the lungs?
Fluid in the lungs or pleural effusion can be caused by heart failure, pneumonia, cancer, kidney disease, or pulmonary embolism. It is important to identify the cause so that you can get proper treatment.
4. Is fluid in the lungs dangerous?
It can be, yes — particularly if left untreated. Beyond the breathing difficulties it causes directly, it often signals an underlying condition that needs attention in its own right.
5. How is pleural effusion treated?
Treatment depends on the cause and severity. It may include medications, draining the fluid through thoracentesis, or treating the underlying disease.
6. What is thoracentesis, and is it painful?
Thoracentesis is a medical procedure used to remove excess fluid from around the lungs using a needle. It’s carried out under local anaesthesia, and most people find it very manageable; discomfort is usually minimal.
7. Can pleural effusion go away on its own?
Mild cases sometimes resolve once the underlying condition is treated. That said, a doctor should always assess it — even a mild effusion can point to something that needs proper attention.
Final Thoughts
Pleural effusion is the body signalling you that something isn’t right. Fluid doesn’t build up around your lungs without a reason, and that reason is almost always worth understanding. The reassuring part is that with the right diagnosis and treatment, whether that’s a simple drainage procedure or targeted care for the root cause, most people recover well and go on to breathe comfortably again.
If anything in this article resonates with what you or someone you know is experiencing, don’t wait. A timely visit to your doctor could be the most important step you take.